

Rainmakers Coming to Old School
|
Thaddeus was a wonderful boy, filled with love and energy, and it was devastating to us when we lost him in January 2016 to complications from a thoracic cyst. The formation of a cyst like this is an extremely rare condition that, according to every vet who consulted on his case, was just a random occurrence that could not be attributed to any real cause (neither genetic, nor congenital, nor environmental --really they have no real idea why he had it). I am sharing his story here in case it may help someone else who may encounter such conditions in their own dog, though based on what I've been told by the vets on Thaddeus' case, that would be extremely unlikely. I first noticed something seriously wrong with Thaddeus in October of 2014 when a short amount of gaiting in the yard left him with what I felt was heavier breathing than he should have had for such a small amount of exertion. Typically he was an extremely active Mastiff who lived to run and jump and play for extended amounts of time without any issues with respiration. I had noticed some coughing after exertion a few months prior which I had believed was kennel cough, but I now suspect the could have been the early warning signs for his condition. Later, the coughing during exertion became much more frequent and I made an appointment with my vet to investigate the cause. I feared it might be a problem with his heart or lungs and braced for bad news. We ran some blood work and did a chest X-ray which revealed... Well what do you see?
A whole lot of something fuzzy. We did an ultrasound to see if we could get more info. The ultrasound revealed a cyst so large the edges couldn't be found. A sample of the cyst was taken by needle aspiration and sent to the lab for cytology. The report we got back wasn't very helpful in guiding us to a course of action to alleviate his breathing symptoms, It suggested more advanced imaging, but both consulting vets indicated that advanced imaging would most likely still not be capable of providing enough information to suggest a treatment course, that only thoracic surgery would provide that information. Here is an excerpt from the first cytology report:
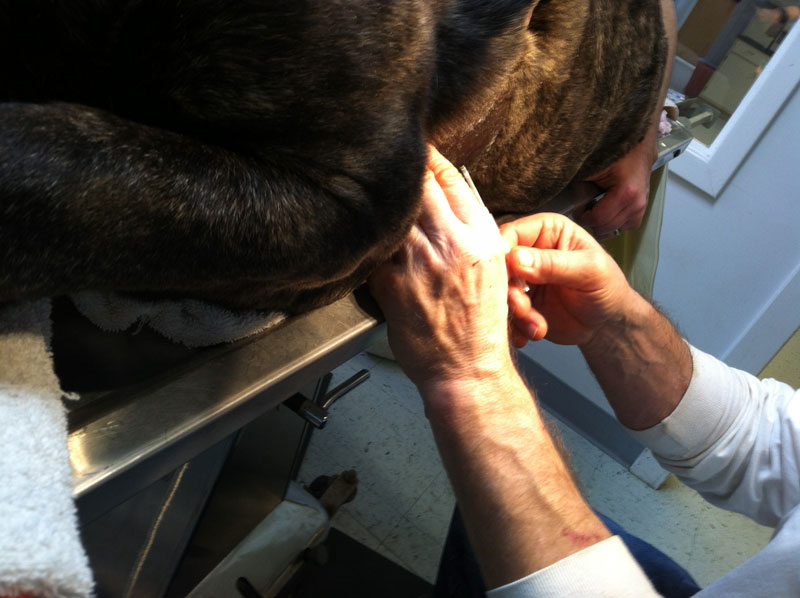
In the end, we opted to attempt to drain the cyst before stepping up to something as dangerous as thoracic surgery. Here is how Thaddeus was breathing the day of his draining, before the procedure: During the procedure it was interesting to see how much higher his oxygen numbers went up on the monitor as the cyst was drained. Ultimately about 2 liters of fluid were drained during the procedure. A photo and video from the draining procedure:
After the draining procedure, Thaddeus was breathing much better and there was hope that he could recover. We also had him on antibiotics and prednisone. Here he is breathing much easier, despite only just waking up from anesthesia.
However, the recovery of breathing function was only temporary and we had to do more draining in October 2015, again getting nearly 2 liters of fluid from his left side of the chest.
|
Again, the recovery of breathing function was only temporary and we had to do yet another draining just a few months later, and this time, we got less fluid, the color of the fluid was darker, the consistency was a little thicker, and the quality of breathing after the procedure was not 100% back to normal as it had been after the previous draining procedures. Another round of blood work showed normal numbers in all areas.
Again, the recovery of breathing function was only temporary and we had to do yet another draining just a few months later, and this time, we got less fluid, the color of the fluid was darker, the consistency was a little thicker, and the quality of breathing after the procedure was not 100% back to normal as it had been after the previous draining procedures. Another round of blood work showed normal numbers in all areas. This is when we decided that we needed to go ahead and take him out to the vet school for a CT scan and probably thoracic surgery. It felt like there was nothing more we could do with the draining, the side effects from the prednisone were getting worse, and his breathing was labored. All through out this, Thaddeus showed no other signs of illness. He was still his normal self, in every other way (appetite, energy level, attitude, etc).
A consultation with The Virginia-Maryland College of Veterinary Medicine (which I will just call Tech for brevity) was scheduled. They re-did his blood work and cytology of the cyst sample, (with very similar results to his earlier tests) they did a CT scan which revealed what exactly we were dealing with, a cyst which nearly completely filled his left chest cavity, covering up almost all indications of lung tissue on that side and even displacing his heart a little.
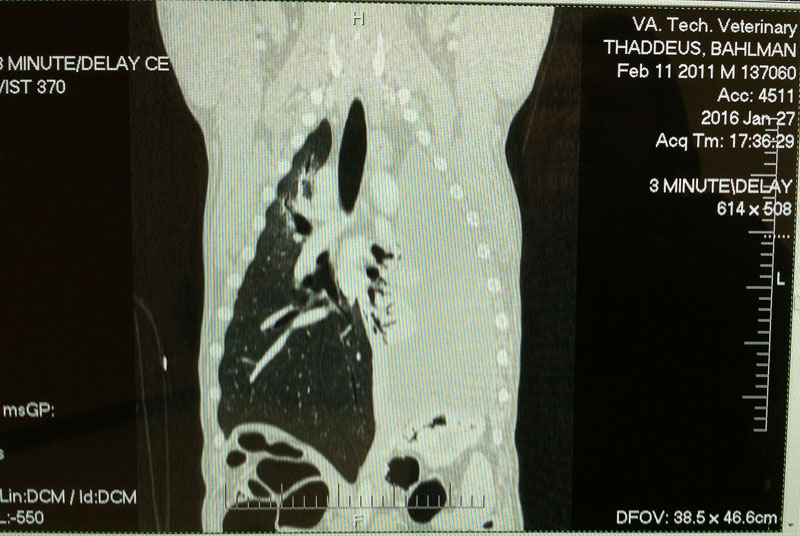
It was recommended we do the surgery, attempt to remove as much of the cyst as possible, more tests would be run on what they removed, they would install chest tubes and monitor his recovery and hopefully in a few days he could go home. They did express that there were many risks involved with the procedure, but that they felt that this was his best chance for attaining a good quality of life going forward and so I opted to do it.
The surgery went fairly well, though they could not remove as much of the cyst tissue as they would have like to have done because it had adhered to the wall of the thorax. He survived the first night and they allowed me to visit him in the ICU the next afternoon. They told me he had to be moved from a larger, horse stall sized enclosure into this crate sized enclosure because he "became agitated" and they were concerned about him pulling his tubes out. He seemed groggy and spacey, and hot, but he was breathing with less effort than before the surgery. I left him feeling a glimmer of hope that he would be getting better.
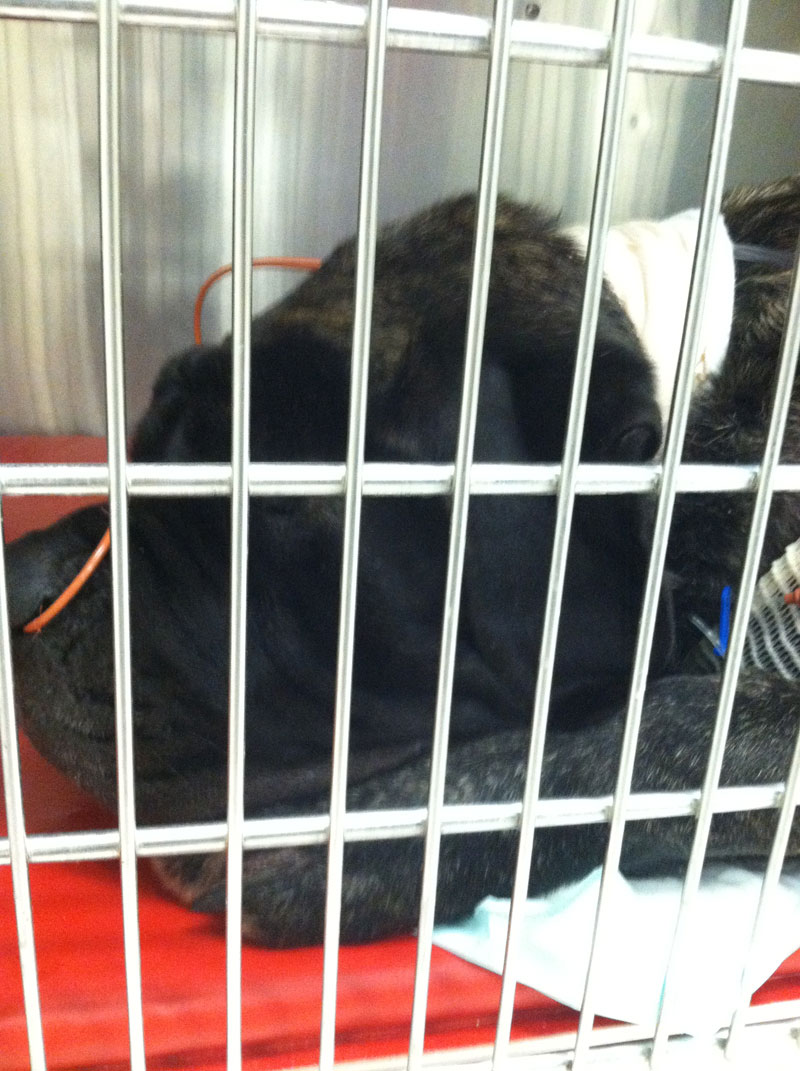



Sadly, that was the last time I saw him. I received a phone call around 2am the next morning notifying me that Thaddeus had gone into cardiac arrest and could not be revived after 30 minutes of trying and should they stop attempts at reviving him. I was shocked because I had believed he was over the worst and was going to recover.
I then waited several weeks for the results of all of the tests they had run before and after the surgery, as well as the necropsy and I will excerpt some of them here.
From the discharge form:
Surgery: On 1/28/16, a median sternotomy was performed. The previously noted mass occupied the entire left hemithorax and was closely adhered to the surrounding tissues (ex. pericardium, diaphragm, pleura, mediastinum). Approximately 2 L dark red fluid was suctioned from the cyst and a large amount of dark reddish brown, soft, friable debris was evacuated from the cyst manually. Within the mass, an approximately 2 cm round white-walled structure containing dark brownish black chalky debris was noted and submitted for histopathology. Samples of tissue from the lymph nodes, mediastinum, and cyst wall were also obtained for histopathology and a sample was submitted for culture/sensitivity. The left hemithorax was copiously lavaged and a left thoracostomy tube was placed prior to closure. No functional lung parenchyma was noted in the left hemithorax at the time of surgery. There were no intraoperative complications noted.
Case outcome: Upon recovery from anesthesia, Thaddeus required oxygen supplementation via bilateral nasal cannulae. He otherwise recovered well and was ambulating nearly normally 12 hours post operatively. He was maintained on multimodal analgesia, including non-steroidal anti-inflammatory drugs, fentanyl and ketamine CRI and low dose dexmedetomidine CRI. He demonstrated agitation which improved with addition of the dexmedetomidine CRI. His cardiovascular parameters were stable and his appetite returned approximately 18 hours post operatively. The thoracostomy tube was aspirated regularly; air production tapered quickly post operatively and fluid production had begun to decrease also. At approximately 1 AM on 1/30/2016, subcutaneous emphysema was noted on the right side of his face with no apparent cause nor change of status prior. Soon after this finding was noted, Thaddeus abruptly went into respiratory arrest and then cardiac arrest. Thaddeus was intubated, his airway suctioned and chest compressions were immediately initiated. Several round of emergency drugs were administered and unfortunately, no return of spontaneous circulation nor respiration was noted. The owner was contacted after initiation of CPR and elected to stop CPR after approximately 30 minutes. The owner elected for a post mortem examination as well as private cremation.
From the necropsy report:
Gross Description
This is a 65kg, 5-year-old intact male Bull Mastiff (sic) dog in good nutritional condition and a fair state of postmortem preservation. Palpable subcutaneous crepitus is present throughout the ventral and lateral neck extending from the thoracic inlet cranially to the mandible; upon dissection this corresponds with extensive subcutaneous emphysema and regions of submandibular edema forming a mass-like effect. Negative pressure is present in the thoracic cavity. Multiple loosely adherent tan fibrillar tags (fibrin) connect the right parietal and visceral pleura and there are multifocal dark red pinpoint foci within the parietal pleura and pericardium (petechiae). The ventral pericardium, cranial mediastinum, left lung lobes, and left parietal pleura are firmly adherent by coalescing fibrous adhesions. Upon removal of the pluck, nearly the entire left lung is covered by a thick, red/brown, firm, undulating plaque (chronic pleuritis). The left cranial lung lobe is distorted and replaced by multiple moderately firm nodular portions of lung, up to 8cm in greatest dimension, that appear to encompass the caudal portion of the left cranial lung lobe. The trachea contains abundant yellow mucoid fluid along its length and this extends into the mainstem bronchi. Bilaterally the retroperitoneal space is distended with air. An unencapsulated, slightly raised, dark purple subcapsular nodule, up to 1.5cm in greatest dimension, is in the caudal margin of the spleen that exudes air and collapses on cut surface. Multiple slightly raised white/tan plaques, 1-2mm diameter, are on the capsular surface of the spleen (siderotic plaques, incidental).
Histologic Description
Spleen: Within the subcapsular red pulp, there are multiple, variably sized, irregularly marginated, unencapsulated air-filled pockets.
Pericardium: The pericardium is diffusely thickened by streams of sparsely cellular collagen line on both surfaces by plaques of fibrin, hemorrhage, and infiltrates of neutrophils and fewer lymphocytes and macrophages.
Lung: Within affected portions of left lung alveoli are nearly completely collapsed and recognizable architecture is obscured by interlacing streams of collagen that replaces alveolar septa. Few macrophages and lymphocytes are present within alveoli and bronchi and bronchioles contain sloughed epithelium and scant mucoid matrix. Bronchi are surrounded by normal cartilage bands. The pleura is diffusely thickened, up to 10 times normal, by dense collagen, scattered aggregates of mineral, hemosiderin laden macrophages, and surface plaques of fibrin and hemorrhage.
Liver, kidney, heart, pancreas, intestine, colon: There are no significant microscopic lesions.
Final Diagnosis
Chronic, severe pleuritis and pleural fibrosis (left hemithorax) and pericarditis Left cranial lung: Regionally extensive pulmonary atelectasis and fibrosis Ventral neck and mandible: Regionally extensive severe subcutaneous emphysema and edema Bilateral retroperitoneal emphysema Spleen: Subcapsular emphysema Multifocal pleural petechiae
Comments
This is a very unusual case. The extensive distribution of emphysema throughout the ventral subcutis of the neck, extending from the thoracic inlet to the mandible, and the retroperitoneum and spleen are nearly identical to the lesions described for experimental induction of pneumothorax following introduction of compressed air into the lung (Joannides M et al. The Etiology of Interstitial and Mediastinal Emphysema. Archives of Surgery, 1929). The major difference, in the present case, is that pneumothorax was not a feature. I suspect this may have been the result of extensive pleuritis and pleural fibrosis within the left hemithorax, which prevented air from escaping through the pleura directly into the pleural space. In the previous reference, even the induction of large volumes of air in the subcutis, thorax, or peritoneum did not cause death. Only the presence of air embolism was fatal, and I suspect that this dog likely died from air embolism stemming from its abnormal lung. Due to the chronicity and extensive fibrosis of the left lung, I am uncertain of the inciting cause of the reported chronic pulmonary cyst. There was no evidence of bronchial cartilage abnormalities to suggest congenital lobar emphysema; rather this may have been the result of a primary bullous emphysema. There is no evidence to suggest that the acute emphysema was related to the previous surgery, though I cannot completely rule out this possibility. There was no evidence of neoplasia in any of the examined sections of lung.
So, take what you will from this story. His vet from Tech told me while explaining these results that they didn't feel the surgery caused the air embolism which caused his death. She said this could have happened to him at any time, due to what his cyst had done to his left lung. Frustratingly, answers about why he had the cyst, and if there had been a better way to handle it have not been answered, though I am grateful to know that it was not genetic and that none of his family members have to worry about this happening to them, and that it was also probably not environmental, so none of my other dogs might come down with this same issue due to some sort of exposure in their environment. I would be happy to go the rest of my life without having to hear a series of vets say to me, "In all my years as a vet I've never seen anything like this." I do wonder if it is possible that it had anything to do with the TPLO surgery he'd had a few years earlier, but the vets seem to think that while this is possible, it's not probable. Even if they were related, there are plenty of dogs who have TPLO surgery without developing this sort of side effect, so I can see why they say that link is not probable.
RIP Thaddeus. I love you and I miss you, and I hope you are chasing balls, sprinklers and toys across the Rainbow Bridge.
| |
|
|
|
|
![]()
Copyright © 2002 to present All Rights Reserved
No photos or text may be reproduced without express written permission.
Site design and hosting by PopularDog.com